Jaw pain can drain your energy, cloud your focus, and strain your sleep. If you live with TMJ pain, you may feel stuck between night guards, pain pills, and worry. Now you may wonder how Botox fits into this picture. This blog explains how Botox can calm overworked jaw muscles and lower TMJ pain. You will see what Botox can and cannot do, how long relief can last, and what risks you must weigh. You will also learn when a Tallahassee dentist may suggest Botox as part of your care plan. The goal is simple. You deserve clear facts so you can talk with your care team and decide what fits your body, your pain, and your life.
What TMJ Pain Really Means
TMJ stands for temporomandibular joint. You have one joint on each side of your face in front of your ears. These joints let you talk, chew, and yawn.
TMJ disorders can cause:
- Aching jaw or face
- Clicking or popping when you open or close
- Locking of the jaw
- Headaches or neck pain
- Ear pressure or ringing
Stress, teeth grinding, joint problems, or injury can all trigger TMJ symptoms. The more your jaw muscles clench, the more the joint hurts. That muscle tension is where Botox may help.
How Botox Works On Jaw Muscles
Botox is a purified protein. Doctors and dentists inject it in tiny amounts into specific muscles. It blocks signals from nerves to muscles. That means the muscle cannot squeeze as hard.
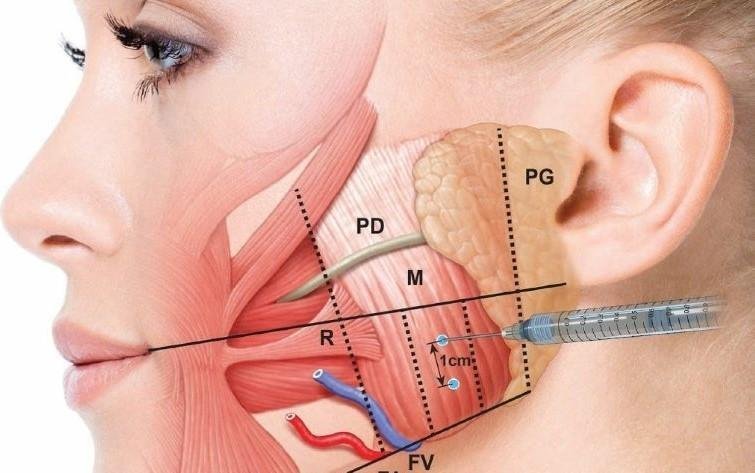
For TMJ pain, Botox is usually placed in three main muscle groups:
- Masseter muscles at the back of your jaw
- Temporalis muscles at your temples
- Sometimes smaller support muscles near the jaw
When these muscles relax, clenching eases. This can drop the constant pull on the joint. Many patients report less pain, fewer headaches, and less wear on their teeth.
The effect is not instant. You may notice change in a few days. Full effect often shows in two weeks. Relief can last three to four months. After that, muscle strength slowly returns. Some people need repeat care to keep pain down.
What Research Shows About Botox And TMJ
Studies are still growing, yet early results show promise for some people. The National Institutes of Health share reviews that describe Botox as helpful for muscle driven jaw pain in select patients.
Key findings across studies include three points.
- Botox can reduce muscle tenderness
- Botox can lower pain scores for many patients
- Results vary and are not permanent
Scientists are still working to learn the safest dose and best injection sites. The U.S. Food and Drug Administration notes that Botox is approved for some conditions like chronic migraine. It is not yet approved for TMJ disorders.
Botox Compared With Other TMJ Treatments
TMJ care usually starts with simple steps. Botox is one choice among many. The table below compares common options.
| Treatment | Main Goal | Pros | Limits
|
|---|---|---|---|
| Night guard or splint | Protect teeth and guide jaw | Noninvasive. Reversible. Used at home. | May not ease strong muscle pain. Needs nightly use. |
| Self care and jaw exercises | Lower strain on joint and muscles | Low cost. You control pace. Supports long term habits. | Needs daily effort. Relief can feel slow. |
| Medicine such as NSAIDs or muscle relaxers | Reduce pain and swelling | Can help flares. Easy to start. | Side effects. Not a long term fix for many people. |
| Botox injections | Relax overactive jaw muscles | Can cut clenching. May lower pain and headaches. | Results wear off. Cost. Possible weakness when chewing. |
| Surgery on the joint | Repair or change joint structure | Can help in severe joint damage. | Invasive. Risks of surgery. Long healing time. |
Who Might Benefit From Botox For TMJ
Botox is not for everyone with jaw pain. You might be a candidate if three things are true.
- You have strong muscle driven symptoms like clenching, grinding, or big masseter muscles
- You tried a night guard, self care, and medicine without enough relief
- Your dentist or doctor rules out other causes like tooth infection or joint disease
Botox may be more helpful when pain comes from muscle overuse and not from joint damage. A careful exam and your history guide this choice.
Risks And Side Effects You Should Know
Every treatment carries risk. Botox is no exception. Possible side effects include:
- Soreness or bruising at the injection site
- Feeling of jaw weakness
- Chewing fatigue, especially with hard foods
- Uneven smile or facial expression in rare cases
- Headache or flu like symptoms
Very rare but serious reactions can occur if the toxin spreads. That is why you must share your health history, medicines, and any nerve or muscle disease with your provider before care.
Questions To Ask Your Dentist Or Doctor
Before you agree to Botox for TMJ pain, ask clear questions.
- What is causing my TMJ pain
- Which muscles will you treat and why
- How much experience do you have using Botox for TMJ
- What relief should I expect in three months
- What will it cost and how often might I need repeat care
- What happens if it does not help
You deserve direct answers. If you feel rushed or brushed aside, seek a second opinion.
How To Support Jaw Health Alongside Botox
Even if you choose Botox, simple daily steps still matter. You can:
- Eat softer foods during flares
- Avoid gum and chewy snacks
- Keep teeth apart when you are not chewing
- Use a night guard if your dentist prescribes one
- Practice stress control with breathing or gentle stretching
These habits protect your jaw and may stretch the benefit of any treatment you choose.
Making A Thoughtful Decision
Botox can give strong relief for some people with stubborn TMJ pain. It can also fall short for others. The choice is personal.
Use three steps to guide yourself.
- Learn the facts about your diagnosis
- Weigh the pros, limits, and risks of each option
- Work with a trusted provider who listens to your goals
Your jaw pain is real. You deserve clear, honest guidance and a plan that respects your body and your daily life.